Boulder Dentist Serving Denver, Ft. Collins & Nearby Areas in Colorado
As a child, Barbara had had a root canal done on her upper right front tooth, tooth #8. Over the years, Barbara had several dental crowns on that tooth but never really liked how they looked. For 45 years, the tooth did not cause any pain until one day she began having pain and pressure especially when chewing. This is when she first sought treatment from Dr. Adler. Based upon the exam, X-rays, and prior history of a root canal, Dr. Adler recommended that Barbara have an apicoectomy.
What Is an Apicoectomy?
An apicoectomy is usually performed after a tooth has had at least one root canal but continues to develop infections. Root canals are very complex, with many small branches off the main canal. Sometimes, even after root canal treatment, infected debris can remain in those branches and possibly prevent healing or cause re-infection later. During Barbara’s apicoectomy, the root tip was accessed directly through the bone instead of up through the tooth as in a root canal treatment. The root tip, or apex, was removed along with the infected tissue. A filling was then placed to seal the end of the root and a suture is placed to close the access opening. In order to stabilize the tooth, Barbara then had an all porcelain crown and carbon fiber post placed.
For a year after the apicoectomy, the tooth was symptom free but unfortunately the tooth became infected again forming an abscess. A tooth or root abscess is pus enclosed in the tissue of the jaw bone at the tip of an infected tooth that usually originates from a bacterial infection that has accumulated in the soft pulp of the tooth. If left untreated, an abscess can continue to grow and may become large enough to perforate bone and extend into the soft tissue. It will continue to follow the path of least resistance and spread either internally or externally which can lead to severe complications. Dr. Adler performed another apicoectomy in an effort to save the tooth hoping that it was another root tip infection. During the procedure, Dr. Adler saw a fracture in the tooth that extending from tip to crown and it was determined that the tooth could not be saved due to the vertical root fracture.
After Tooth Extraction

The tooth was extracted and a bone graft, allograft, was placed to help replace the bone that had been lost due to the abscess. A removable temporary partial, custom made prior to the appointment, was fitted so that Barbara was able to leave the office without a gap in her smile while she continued to heal.
While the graft was healing, Dr. Adler was able to perform guided tissue recontouring.
Guided tissue recontouring reshapes the gum around the tooth giving a more aesthetic look. This was done for Barbara by slowing adding material to tooth on the temporary partial where it presses against the gum line. Overtime the tissue is gently formed into the desired shape to better match the other teeth.
Placing the Implant
Once the graft had healed and become stable, we placed the titanium implant. The implant was placed during a surgical procedure, directly into the jawbone and under the gums. The implant with a healing cap attached was then allowed to heal for four to six months so that the bone will grow around the implant and "osseo-integrate".
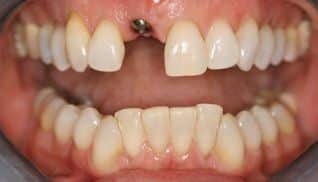
We later placed a soft tissue graft because Barbara needed more connective tissue to support the implant.
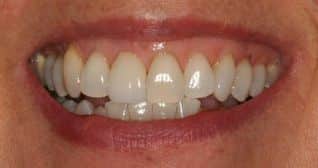
After six months of healing, Dr. Adler placed a zirconium implant post, also known as an abutment, that connected to the implant. The post was made of zirconium to allow for ideal translucency once the all porcelain crown was place about a month later. So today, Barbara is no longer bothered by that troublesome tooth and she looks great.
Dr. Adler's Patient Excited with Her New Smile

"Adler Dentistry is super proactive in their approach to dental care. The staff is super friendly and organized. I went in for a filling and was done within 20 minutes!"